| Literature link | GPT Summary | Evidence category | Disease type |
|---|---|---|---|
| 24912095 | This study assessed whether an early hemoglobin A1c (HbA1c) value of 5.7–6.4% could predict the progression to gestational diabetes mellitus (GDM). Among women screened before 20 weeks of gestation, 27.3% of those with HbA1c levels of 5.7–6.4% developed GDM, compared to 8.7% with HbA1c <5.7% (odds ratio: 3.9; adjusted odds ratio: 2.4). The increased risk remained significant after adjusting for multiple confounders. However, no significant differences were observed in maternal weight gain, delivery route, birthweight, or neonatal morbidities between the groups. The findings suggest that women with an HbA1c of 5.7–6.4% should receive closer monitoring and potential early intervention for GDM prevention. |
Risk factor |
GDM |
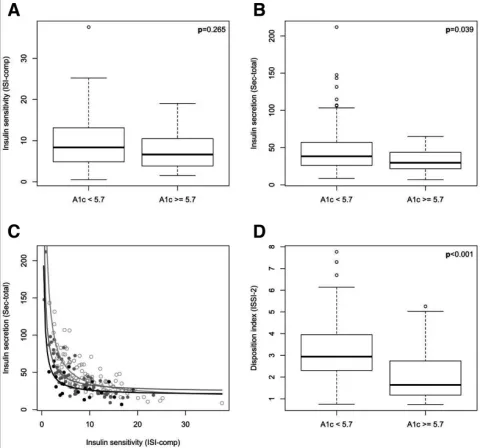
| 33132213 | This study evaluated the potential of hemoglobin A1c (HbA1c) as an early screening tool for identifying women at risk for gestational diabetes mellitus (GDM). Among 220 pregnant women tested at 16 weeks gestation, an HbA1c ≥5.7% (39 mmol/mol) was associated with altered glucose dynamics, impaired beta-cell function, and delayed glucose peak during an oral glucose tolerance test (OGTT). The HbA1c cutoff of 5.7% demonstrated high specificity for GDM diagnosis (0.96) and glucose-lowering treatment need (0.95), though its overall predictive accuracy was moderate. Elevated HbA1c was also linked to an increased risk of delivering large-for-gestational-age infants, independent of GDM status. These findings suggest that early HbA1c measurement reflects underlying glucose intolerance and beta-cell dysfunction, supporting its utility in early risk stratification for GDM. |
Risk factor |
GDM |
| 25190675 | This study investigated the optimal HbA1c threshold for detecting undiagnosed diabetes in early pregnancy and its association with adverse pregnancy outcomes. Among 16,122 women tested at a median of 47 days' gestation, an HbA1c ≥5.9% (41 mmol/mol) identified all diabetes cases detected by an early oral glucose tolerance test (OGTT) performed before 20 weeks, including those with HbA1c below the standard 6.5% (48 mmol/mol) cutoff. Women with HbA1c levels of 5.9–6.4% had significantly increased risks of major congenital anomalies, preeclampsia, shoulder dystocia, and perinatal death compared to those with HbA1c below 5.9%. The findings suggest that HbA1c ≥5.9% in early pregnancy is a practical and effective marker for identifying women at high risk of diabetes and adverse outcomes, emphasizing its value for early intervention. |
Risk factor |
GDM |
| 31794807 | This study assessed the efficacy of first-trimester glycated hemoglobin (HbA1c-FT) in predicting gestational diabetes mellitus (GDM) among Asian Indian women. In a cohort of 2,275 women, those with GDM had a significantly higher mean HbA1c-FT (5.04% vs. 4.9%, p < 0.001). Women with HbA1c-FT levels of 5.2–5.5% and >5.6% had an increased adjusted odds ratio for GDM of 1.627 (p < 0.004) and 2.6 (p < 0.001), respectively, compared to those with HbA1c-FT <5.2%. Although HbA1c-FT was identified as an independent predictor of GDM, its area under the ROC curve (0.606) indicated insufficient sensitivity and specificity for it to serve as a standalone diagnostic test. |
Risk factor |
GDM |
| 26351946 | This study aimed to develop a predictive model for early identification of gestational diabetes mellitus (GDM) based on clinical factors and biomarkers. Using data from a cohort of 7929 pregnant women, a nested case-control analysis was conducted, including 264 women with GDM and matched controls. HbA1c and hsCRP were elevated, while SHBG was reduced in women who developed GDM (p<0.001). The predictive model for GDM, incorporating HbA1c, SHBG, BMI, history of GDM, family history of diabetes, and pre-pregnancy soft drink intake, achieved an AUC of 0.79. For predicting GDM requiring insulin therapy, the model had an AUC of 0.88 and a sensitivity of 68.9% at a 10% false-positive rate. This simple model could enable early identification of women at risk of GDM, particularly those requiring insulin therapy, facilitating timely interventions. | Risk factor | GDM |
| KEGG pathway |
|---|
| African trypanosomiasis, Malaria |
RF's name
Hemoglobin A1c
RF's type
Complete blood count